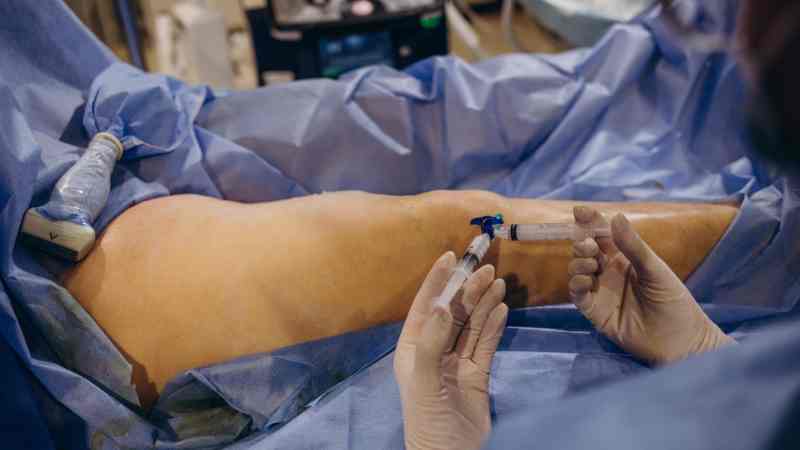
As a Chicago native and a successful North Suburban transplant, I’m a vein doctor that has seen some pretty significant changes happen around Chicagoland over the years. But all of the political, socioeconomic and demographic changes pale by comparison to the significant technological breakthroughs that have rolled into town over the past decade.
The history of varicose vein treatment options reads much like politics in Chicago. Things just kept getting done the same way that they have always been done because that is how things get done. Sounds like a quote from the late mayor, Richard J. Daley, right?
Well, Hizzoner‘s advice included, “Don’t make no waves and don’t back no losers”. For years, the status quo in varicose vein treatment favored surgical stripping…involving general anesthesia and a prolonged and painful recovery period. Not only that, the rate of recurrence approached 40%. Sounds like a loser to me. Sounds like some waves needed to be made[<– subtle foreshadowing]…
Then a rogue wave hit more than 10 years ago: endovenous thermal ablation. It was a game-changer:
+ an outpatient procedure using only local anesthesia
+ quick recovery
+ essentially no down-time
+ Recurrence rate in the single digits.
So…Why isn’t everyone with superficial venous insufficiency having such minimally-invasive procedures done?!
Well, the only reason I can think of is that they and their primary doctors are unaware of what is currently the state-of-the art treatment modality for varicose veins. I‘m here to change all that.
We will talk more of endovenous thermal ablation shortly. For now, let’s discuss the Conservative Management of Superficial Venous Insufficiency:
The mainstays of conservative management of venous disease of the lower extremities includes the “6 E’s”:
Exercise: 5-30 minutes a day if possible
-Strengthens your “peripheral heart”
-Calf muscle pump becomes more efficient
-Most patients notice a significant decrease in symptoms within a few weeks
-Basel Study: Way back in 1978 when other Baselites were partying to the Disco sounds of The Bee Gees, Dr. Widmer and colleagues nerded their nights away by studying the effects of lack of movement on leg veins…and G-d bless ’em for doing it! They found that a decreased amount of daily movement was associated with an exponential increase in the prevalence of venous disease. So…stay active. Consider disco dancing. Or not.
Elevation of legs: Find your favorite way to keep your feet above the level of your heart for 15-30 minutes twice daily.
Eat right: even moderate weight loss may reduce symptoms
Emollients: If you’ve reached the point where skin changes have occurred, such emollients may decrease cracking/fissuring as well as treat dermatitis.
Eschew (avoid) High Heels:
Wearing them decreases the full pumping action of calf muscles→decreases venous emptying of your leg veins→increased symptoms.
External Compression:
In general bandages/stockings that compress the legs have some important properties that may improve venous disease. They include:
–Decreasing the diameter of veins. This increases the flow velocity through veins and decreases the chances for clots to develop within them
–Acts against filtration of fluid out of veins and into tissues, thereby decreasing edema
–Improves the function of the calf “pump”
–Decreases reflux within veins with incompetent valves
-Most interestingly, scientists have documented a decreased inflammatory response in legs treated with external compression.
– Nowadays, many athletes wear compression stockings/sleeves/garments. Some data suggests that doing so may decrease recovery time after strenuous activity.
External compression comes in a few flavors. Namely, inelastic, elastic and pneumatic.
Inelastic: scientifically better but less practical (another way of saying fashion backward).
Better because:
-Creates a rigid envelope around the leg→full force of the calf muscle is directed inward
-No elastic recoil/compression during rest→ no interference of influx to the deep system
Elastic: Graduated Compression
If fitted properly:
-100% of the stated pressure is delivered at the ankle→70% at the calf→40% at the thigh
–Creates a gradient where flow is directed up and out of the leg.
Improperly fitted: Can create a “tourniquet effect”
-Favors blood flow back down the leg→BAD
Over-the-counter stockings are typically 8-15mmHg of pressure. Patients need prescription-strength with at least 20-30mmHg to have any meaningful results.
Pneumatic: Intermittent pneumatic compression
Some of you may have experienced such devices while in the hospital. These are the contraptions that are velcroed around patient’s legs and then intermittently fill up with air in a sequential way going up the leg. Patients can rent or buy such devices for home use. People may typically do so if their compression stockings alone don’t work.
All-in-all, for patients with significant reflux in their superficial venous system, compression treatment alone won’t solve their problem. It isn’t definitive treatment. However it really remains the cornerstone to treating venous disease because no matter what treatment modality is ultimately chosen, patients will still need to wear them:
-Before definitive treatment
-After treatment:
-I typically have patients wear them during the 1 week post endogenous ablation period
-After sclerotherapy, patients wear them during the daytime and continue to do so until around 1 month after the final treatment is performed.
–In order to fulfill the requirement of insurance carriers, patients need to demonstrate that they have tried conservative treatment with compression stockings for some weeks to months, depending on individual insurance companies (Check your policy for details).
The bottom line is that the more you wear compression stockings, the better your outcome will be in the long run.
So thus ends our talk of the conservative management of venous disease. It must be stressed that no matter how effective such measures are at relieving symptoms, NONE OF THEM WILL FIX THE UNDERLYING PROBLEM…namely, faulty vein valves. For that, an intervention is needed to actually or effectively disconnect the bad veins from the rest of the venous system. This will be the topic discussed in my next post, G-d willing.
Meanwhile, if you have further questions and would like to consult with me further regarding your particular issues, please call 847-272-8346. to schedule your initial consultation.
I look forward to seeing you and helping to make your legs feel and look better than they have in years!